In This Article
Hallux Valgus is a condition that affects the big toe joint. It causes thickening of the joint and turns the big toe inwards, towards the other toes.
This condition of the big toe joint (known as 1st MTP) usually has pain and swelling around the joint as part of its symptoms.
(It’s also referred to as a “Bunion” – for more info on bunions, see our post here.)
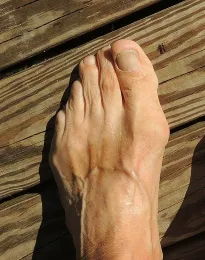
The bump you see here, and the way the big toe tilts towards the smaller toes, is the condition known as Hallux Valgus.
As the joint is subject to strong and sustained forces, it reacts and thickens up.
As it thickens, the new bone formation causes the joint to change axis and angle inwards.
The reason Hallux Valgus tends to progress over time (without suitable management strategies) is that, as it angles, it becomes more vulnerable to overload, which in turn speeds up the condition.
But Hallux Valgus, or Bunions, are the subject of a lot of myths and rumours. We’ll cover them all below, but a few common ones are:
- You inherited your bunions from your mother
- Bunions are caused by pointy shoes and high heels
- Bunions aren’t reversible, they’ll get worse quickly and there’s nothing you can do
All of these myths are true in a small part, but the message has been lost and the key point of each isn’t what you think it is.
The best news is that the earlier you correct the cause of your hallux valgus, the better the outcome.
It might be as simple as choosing a different type of shoe (no, not ugly “old people” shoes!)
If you wanted to skip to our Physiotherapist’s recommendations on the best shoes for bunions, click here.
Myth 1: you inherited bunions from your mother
Genetics are not solely responsible for bunions, but they do contribute.
Hallux Valgus is a condition caused by poor foot stability (excessive pronation which causes a rapid collapse of the arch).
That arch collapse forces the big toe sideways under immense force, creating the reaction that causes bunions to form over a period of years and decades.
Your parents didn’t cause your arch to roll inwards, but they did give you the bone structure that make up your feet.
Some feet aren’t well shaped for stability, so your genetics can make it a more difficult task to resist pronation.
Truth: genetics can make it harder to stabilise the foot, and foot stability is the main cause of Hallux Valgus. So you didn’t inherit bunions from your mother but she may have given you less-than-ideal foot biomechanics which can contribute to Hallux Valgus.
Myth 2: Bunions are caused by pointy shoes and high heels
This is one of my favourites – high heels shoes and pointy shoes will force your toes inwards and the big toe stays angled.
How weak must our joints be if the force of a tight shoe can permanently disfigure a joint?!?
In reality, the toe joints are super strong and a brief bending of the toe might cause soreness for a few days but not much else.
The force of a tight toe isn’t enough to cause a bony reaction and joint changes. Otherwise we could just pull our flimsy joints the other direction and straighten it up again.
The forces required to cause Hallux Valgus are very large, and sustained for a long period of time.
It takes your whole body weight leveraging on the big toe joint, combined with poor alignment, and happening over and over for decades to cause this joint to change shape.
The process is a combination of bony alignment (from previous fractures or genetics, discussed above), rapidly increasing or excessive body weight and footwear selection, which all contribute to biomechanical overload of the joint.
Truth: high heels will make maintaining good foot stability difficult. But we’re usually not walking in them long enough to created the sustained force needed to change the joint. Pointy shoes might bend the toe sideways but it’s not even close to enough force to contribute to bunions.
Myth 3: Bunions aren’t reversible, they’ll get worse quickly and there’s nothing you can do
This one is true in part, but it’s not as doom and gloom as it sounds.
Yes, Hallux Valgus/Bunions are not reversible. They don’t self-correct or go away with time.
Yes, they often get worse over time. But it’s not a quick process depending on your causes and the stage of the condition.
If it’s early days for your bunions, they progress very slowly over a period of decades.
If the cause is poor footwear choices, it’s as easy as getting better shoes to significantly slow the progression of the condition.
Which brings us to “there’s nothing you can do about it” – unfortunately this happens, but it’s only true in the worst cases and at the very last stage of the condition.
With decades of worsening Hallux Valgus, it can get to a stage when the toe is so angled (think 60 degrees or more) that the only option is surgery.
For everyone else though, there’s plenty of very effective options to manage the condition and get rid of the symptoms.
The public perception of bunions and the “there’s nothing you can do” statement often comes from a well-meaning friend that knows someone with a late stage condition who is struggling to walk. It’s the only advice they’ve ever heard because no-one speaks to friends about their mild, very treatable bunions. So the public perception is biased by the horror stories without a balanced point of view.
Truth: The condition is progressive and not reversible (although it can be corrected with surgery) but the rate of progress can be slowed significantly with treatment and footwear and there’s almost always something you can do to help them.
The most effective treatments
Shoe selection is vital to slow the progression of the condition – see our recommendations of the “Best running shoes for bunions“.

Shoes should have adequate room around the toe area and offer some support to assist control of pronation.
Supportive sandals can be a good option, so long as the supporting straps don’t put pressure on the big toe joint.
See the image – the forefoot strap on the Right foot is pushing the foot back in the shoe as it squeezes on the bunion.
Stability exercises in loaded/weight-bearing positions help control the foot position and reduce excessive load on the big toe joint.
Soft orthotics can provide rapid relief of soreness and assist in minimising flare ups with exercise.

Comments are closed.